Silica Dust and the Resurgence of Black Lung Disease: A Crisis for Appalachian Coal Miners Amidst Regulatory Delays and Federal Policy Shifts


Justin Smarsh, a 42-year-old resident of Cherry Tree, Pennsylvania, spent his youth navigating the rugged terrain of the Appalachian Plateau. High above the riverbeds northeast of Pittsburgh, Smarsh was an avid outdoorsman who taught his sons to hunt in the same woods where he had spent his own childhood. Today, those activities are memories of a former life. Smarsh describes a sensation of "suffocation" that accompanies even the most mundane tasks, such as walking across a room or bending down to tie his shoes. He is plagued by a persistent dry cough, the outward symptom of a terminal internal decay.
A third-generation miner, Smarsh followed his father and grandfather into the coal seams of his home county shortly after marriage. In a region where economic opportunities are often sparse, the mines offered the highest-paying wages available. However, the cost of that paycheck has manifested as progressive massive fibrosis (PMF), the most advanced and lethal form of coal workers’ pneumoconiosis, commonly known as black lung disease. There is no cure for PMF. Smarsh manages his condition with a regimen of medications designed to slow the inevitable progression toward heart failure or respiratory collapse. His physicians have provided a stark prognosis: he is unlikely to see his 50th birthday.
The experience of Justin Smarsh is increasingly common across the Appalachian coal belt, contradicting the popular narrative that coal mining and its associated health risks are relics of the industrial past. According to Deanna Istik, CEO of Lungs at Work, a specialized clinic in Washington County, Pennsylvania, the region is witnessing a diagnostic surge. "We see more people being diagnosed with black lung disease than we ever have before," Istik noted, highlighting a public health crisis that is accelerating even as the industry itself faces a complex economic future.

The Shift from Coal to Stone: The Silica Factor
The primary driver behind this modern epidemic is not coal dust alone, but a more aggressive pulmonary irritant: crystalline silica. Historically, miners worked large, thick seams of coal that required minimal disturbance of the surrounding rock. As these primary seams have been exhausted over decades of intensive extraction, modern mining operations must cut through significant layers of quartz-rich sandstone to reach smaller, thinner coal deposits.
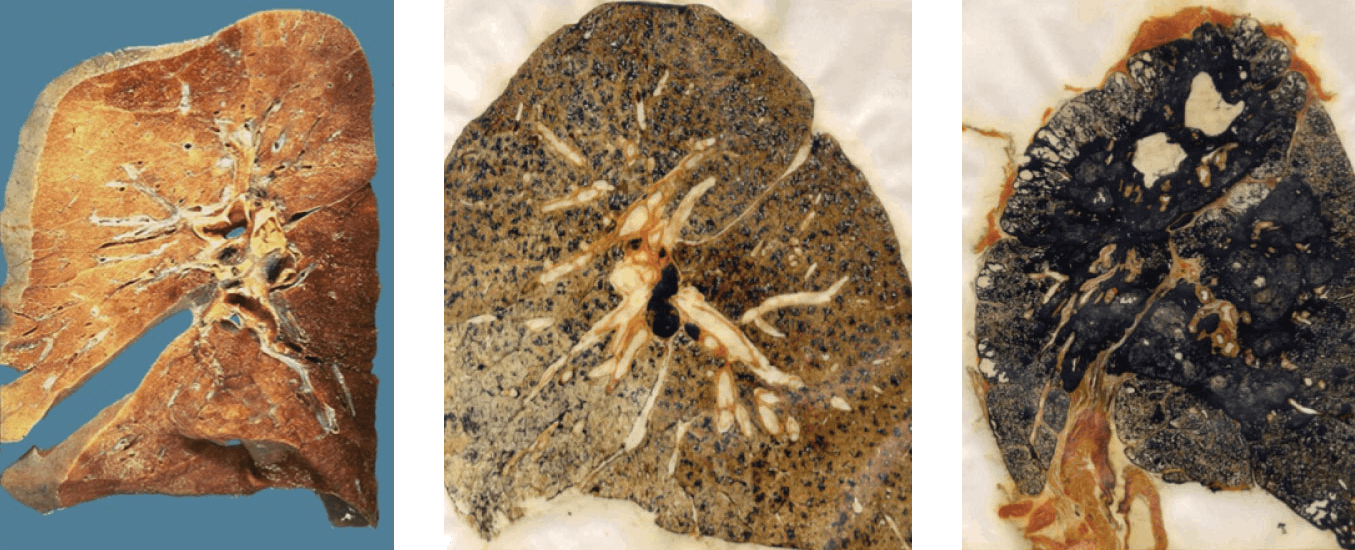
When mining machinery pulverizes this rock, it releases microscopic particles of crystalline silica. Unlike coal dust, which triggers the formation of nodules and scar tissue over decades, silica particles act as microscopic shards of glass. Once inhaled, they cause rapid, severe inflammation and irreversible tissue scarring. This "accelerated silicosis" leads to the development of PMF much faster than traditional black lung. Researchers from the National Institute for Occupational Safety and Health (NIOSH) estimate that PMF now afflicts approximately one in ten miners who have spent at least 25 years underground.
The epidemiological data is alarming. Between 2013 and 2017, hundreds of advanced PMF cases were identified at just three clinics in Virginia, prompting NIOSH to declare a renewed black lung epidemic. While black-lung-related mortality showed a downward trend between 1999 and 2018, that progress has reversed; deaths associated with the disease rose significantly between 2020 and 2023.
A Chronology of Regulatory Failure and Industry Resistance
The struggle to regulate mine safety in the United States has a long and often tragic history. Black lung was not officially recognized as an occupational illness until the late 1960s, following the Farmington Mine disaster in West Virginia that claimed 78 lives. The subsequent 1969 Coal Mine Health and Safety Act established the first federal safety inspections and a benefits program for afflicted workers. These standards were largely successful, nearly eradicating the disease by the late 1990s.

However, the emergence of silica dust has rendered those older standards obsolete. The timeline of the current regulatory battle reflects a decade of administrative friction:
- 1970s: NIOSH first suggests a silica exposure limit of 50 micrograms per cubic meter of air.
- 2016: The Occupational Safety and Health Administration (OSHA) adopts the 50-microgram standard for general industry and construction.
- 2017: The Mine Safety and Health Administration (MSHA), facing industry lobbying, maintains a more lenient limit of 100 micrograms for miners.
- 2024: Following years of advocacy from groups like the Appalachian Citizens’ Law Center, MSHA announces a final rule to lower the limit to 50 micrograms, with enforcement scheduled for April 2025.
- April 2025: Just days before enforcement was to begin, the 8th U.S. Circuit Court of Appeals grants an emergency stay. Simultaneously, MSHA announces an indefinite delay to allow operators more time for compliance.
This indefinite delay has drawn sharp criticism from labor advocates. Rebecca Shelton, director of policy for the Appalachian Citizens’ Law Center, characterized the delay as a political maneuver that prioritizes industry timelines over human lives. "They are hiding behind a ridiculous legal process to delay action while miners get sick and die," Shelton stated.
The Political and Economic Tug-of-War
The regulatory stalemate occurs against a backdrop of aggressive federal support for the coal industry. The current administration has reaffirmed coal as a cornerstone of national security, directing billions of dollars toward coal projects and infrastructure. In late 2023, the Department of Energy announced a $625 million investment in coal-related ventures.
While the administration promotes the "rebirth" of coal, the agencies tasked with protecting workers have seen their capabilities eroded. MSHA’s coal mine enforcement staff has been reduced by approximately 50 percent over the last decade. Furthermore, recent federal buyout programs—referred to as the "Fork in the Road"—led to the departure of 7 percent of the agency’s full-time workforce in a single year. Job offers for 90 newly hired inspectors were also rescinded, leaving a vacuum of expertise at a time when the implementation of new silica rules requires rigorous oversight.
Industry groups, including the National Mining Association (NMA) and the National Stone, Sand & Gravel Association, have argued that the new silica standards are technically unfeasible for some operations. Their legal challenges suggest that when ventilation systems (engineering controls) fail to meet the 50-microgram limit, companies should be allowed to rely on respirators to achieve compliance.
Advocates and medical professionals, however, argue that respirators are an insufficient "last line of defense." Deanna Istik points out that silica particles are so small they can penetrate many standard masks, especially in the hot, humid, and high-exertion environment of an underground mine. Smarsh corroborated this, noting that while he wore a respirator when possible, the physical demands of his job as a roof bolter often made it impossible to maintain a proper seal or breathe adequately through the device.
Regional Impact and the Generational Cycle
Despite the national decline in coal production—which fell from 1,170 million tons in 2008 to 578 million tons in 2023—coal remains a vital economic pillar in Pennsylvania. A 2024 report by the Pennsylvania Coal Alliance indicates that the industry still supports over 5,000 direct mining jobs and generates $2.2 billion in economic output for the state.
This economic dependence creates a culture of silence. Many miners are reluctant to seek medical testing for fear that a diagnosis will lead to termination or industry blacklisting. "I think there’s always going to be that fear of retribution," Istik said. This fear often results in miners working until their lung function is so compromised that they are forced into emergency medical care.

For families like the Smarshes, the tragedy is compounded by a lack of alternatives. Justin Smarsh’s 19-year-old son is currently considering a career in the mines, drawn by the same high wages that attracted his father. Smarsh finds himself in the painful position of warning his son against the only stable career path in their community.
"Me and my wife tell him all the time, ‘You see what I’m going through?’" Smarsh said. He noted that the "good coal" is gone, leaving only the dangerous rock and silica behind. His disillusionment with the industry is total, viewing the current regulatory delays as a sign that corporate profits remain the priority. "They say they care about miners, but you go underground, you’re taking the risk… to fill their pockets full."
Broader Implications for Public Health
The resurgence of black lung and the rise of silicosis represent a significant burden on the U.S. healthcare system and the Black Lung Disability Trust Fund, which provides compensation to miners when their former employers have gone bankrupt. As more miners in their 30s and 40s are diagnosed with PMF, the long-term costs of lung transplants, oxygen therapy, and disability payments are expected to soar.
The current legal and administrative limbo regarding the silica rule leaves thousands of workers in a state of vulnerability. Without the enforcement of the 50-microgram standard and the required engineering controls, experts warn that the current "epidemic" will only widen. For Justin Smarsh and others like him, the debate over micrograms and administrative stays is an abstract battle with a very concrete ending. As the industry looks toward a subsidized future, the men responsible for extracting the "black gold" continue to pay with their breath.







