A Novel Approach to Sepsis Treatment Targets a Key Protein in Blood Plasma
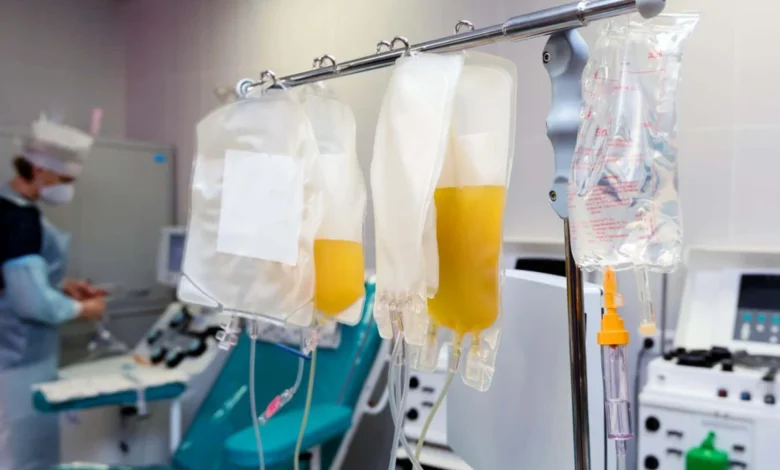
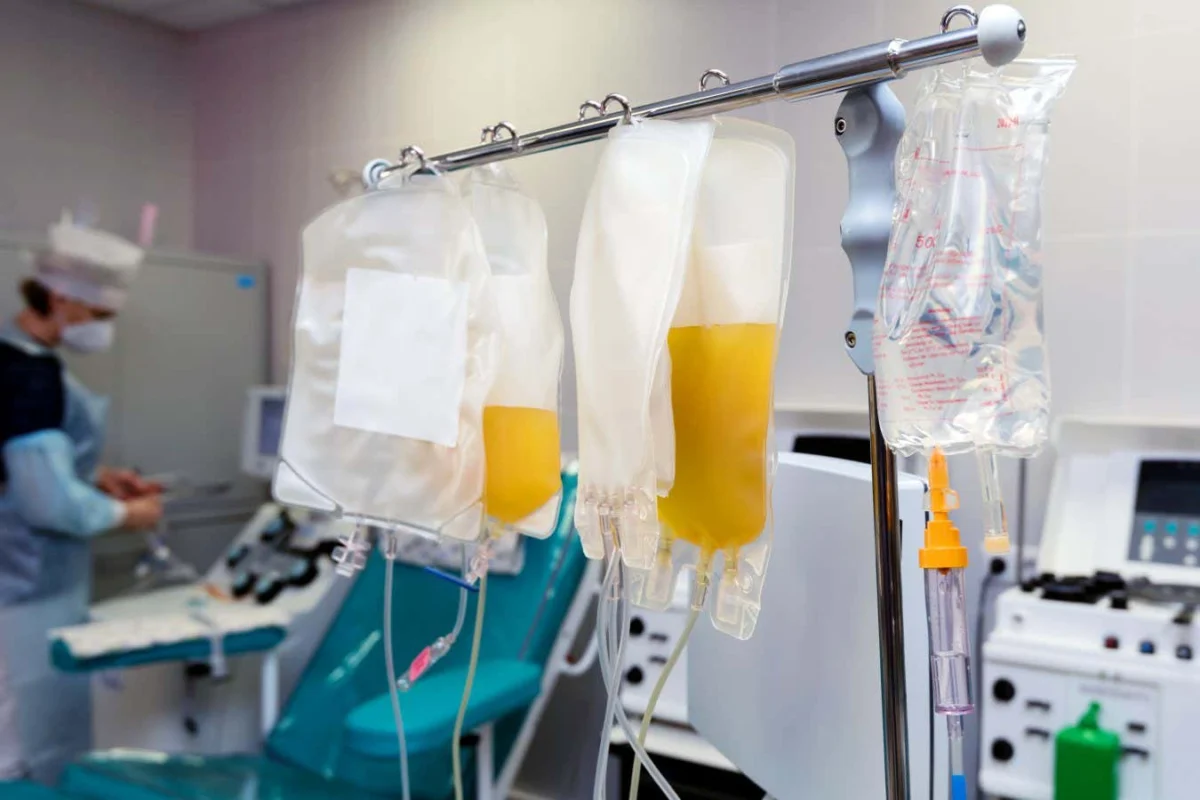
The relentless fight against sepsis, a life-threatening condition that claims millions of lives globally each year, may soon see a significant advancement. Researchers are developing an innovative treatment that involves filtering a patient’s blood to specifically remove a protein, galectin-3, which is believed to be a major driver of the body’s destructive immune overreaction. Early promising results from animal models suggest this novel apheresis technique could dramatically improve survival rates, with human trials slated to begin as early as 2027.
Sepsis represents a critical medical emergency, arising when the body’s own immune system, in its attempt to combat an infection, unleashes a cascade of inflammatory responses that inadvertently damage healthy tissues and vital organs. This overwhelming immune assault can rapidly progress to septic shock, a state of profound circulatory collapse characterized by a dangerous drop in blood pressure. The global burden of sepsis is staggering; a landmark 2017 study estimated a chilling 49 million cases worldwide. Subsequent analyses, including a comprehensive meta-analysis of patients across Europe, North America, and Australia, revealed a grim mortality rate: 32 percent of individuals diagnosed with sepsis succumbed within 90 days of diagnosis. For those afflicted with septic shock, this figure escalated to a harrowing 39 percent, underscoring the urgent need for more effective therapeutic interventions, even with existing treatments for the initial infection and organ support.
Unveiling the Role of Galectin-3
At the forefront of this potential breakthrough is Dr. Isaac Eliaz, a researcher at the Amitabha Medical Clinic and Healing Center in Santa Rosa, California. Dr. Eliaz has dedicated decades to unraveling the complex biological functions of galectin-3. In healthy individuals, this versatile protein plays a crucial role in fundamental cellular processes, including the regulation of cell growth, division, and programmed cell death (apoptosis). It also contributes to the activation and modulation of immune cells. Due to its widespread involvement in cellular regulation, galectin-3 has been implicated in a broad spectrum of diseases, ranging from autoimmune disorders to various forms of cancer. "It covers a whole array of diseases, from autoimmunity to cancer," Dr. Eliaz stated, highlighting its pervasive influence.
This extensive involvement in diverse pathologies naturally led Dr. Eliaz to investigate whether galectin-3 might also play a detrimental role in the context of sepsis. His hypothesis gained traction as multiple studies began to demonstrate a clear correlation between elevated levels of galectin-3 in patients with sepsis and an increased risk of mortality. These findings provided a critical foundation for exploring therapeutic strategies aimed at mitigating the impact of this protein.
The Galectin-3 Apheresis Technique: A Detailed Look
Building on this understanding, Dr. Eliaz and his team conceptualized and developed a specialized apheresis device designed to selectively extract galectin-3 from a patient’s bloodstream. The procedure involves a sophisticated process:
- Blood Withdrawal: A small volume of the patient’s blood is carefully drawn and channeled into the apheresis system.
- Cellular Separation: The collected blood is then subjected to centrifugation, a process that spins the blood at high speed to separate its components. This effectively isolates the cellular elements (red blood cells, white blood cells, and platelets) from the liquid plasma.
- Targeted Protein Removal: The separated plasma, containing various proteins including galectin-3, is then directed through a unique filter. This filter is engineered with specific antibodies that have a high affinity for galectin-3. As the plasma flows through, these antibodies bind to and capture the galectin-3 molecules, effectively removing them from the liquid.
- Reinfusion: Once the galectin-3 has been removed, the purified plasma is recombined with the patient’s original blood cells. This mixture is then safely returned to the patient’s circulation.
This method, known as therapeutic apheresis, offers a targeted approach to modulating the biochemical environment within the body, potentially halting or reversing the damaging effects of excessive galectin-3.
Pre-Clinical Validation: Promising Results in Animal Models
The efficacy and safety of this galectin-3 apheresis device have undergone rigorous testing in pre-clinical studies, notably by a research team led by Dr. Zhiyong Peng at the Zhongnan Hospital of Wuhan University in China. Their comprehensive investigation employed a multi-faceted approach to validate the hypothesis and assess the therapeutic potential of the technology.
Human Blood Analysis: The study commenced by analyzing blood samples from 87 patients diagnosed with sepsis and 27 healthy volunteers. The findings corroborated previous research, revealing significantly higher levels of galectin-3 in the blood of individuals with sepsis compared to the healthy control group. Crucially, among the sepsis patients who survived, a notable decline in galectin-3 levels was observed, further strengthening the link between the protein and disease outcome.
Rat Model of Sepsis: To evaluate the therapeutic impact, the researchers utilized a rat model of sepsis induced by puncturing the large intestine. A total of 48 rats developed sepsis. Of these, 28 underwent galectin-3 apheresis, while the remaining 20 received a sham procedure, designed to mimic the process without the targeted protein removal. The results were striking: 57 percent of the rats treated with galectin-3 apheresis survived, a significant improvement compared to the mere 25 percent survival rate in the control group. This demonstrated a clear survival benefit associated with the targeted removal of galectin-3.
Miniature Pig Model of Sepsis: Further validation was sought using a miniature pig model, known for its physiological similarities to humans. Sepsis was induced in these animals by administering lipopolysaccharide (LPS), a potent component of bacterial cell walls that triggers a robust immune response akin to that seen in severe infections. The pigs were managed with standard intensive care unit protocols. Sixteen pigs received galectin-3 apheresis, while 15 underwent a sham apheresis procedure. Once again, the results favored the therapeutic intervention. The survival rate in the galectin-3 apheresis group was 69 percent, a substantial increase from the 27 percent observed in the sham apheresis group. The consistency of these positive outcomes across two distinct animal models provides robust evidence for the potential efficacy of this novel treatment.
Expert Perspectives and Future Directions
The promising findings have garnered attention from leading experts in critical care and sepsis research. Dr. Djillali Annane, a distinguished researcher at the Raymond Poincaré Hospital in Garches, France, acknowledged the innovative nature of the approach. "This is innovative, for sure," Dr. Annane commented. "The results are consistent in the two animal models."
However, Dr. Annane also emphasized the considerable journey ahead before galectin-3 apheresis can be considered for routine clinical use. He highlighted the need for a deeper mechanistic understanding of precisely how galectin-3 contributes to the pathogenesis of sepsis at a molecular level. Furthermore, he underscored the importance of independent replication of these findings by other research groups and the necessity of testing the treatment in a wider range of animal models, including primates, to further assess its safety and efficacy.
The Road to Human Trials and Broader Implications
Dr. Eliaz’s company, Eliaz Therapeutics, is actively pursuing the necessary funding to initiate a randomized clinical trial in human patients. The company aims to commence this crucial trial in 2027. Such a trial would involve comparing the outcomes of patients receiving galectin-3 apheresis with those receiving standard care or a placebo, providing definitive evidence of its clinical benefit.
The potential implications of a successful galectin-3 apheresis therapy are profound. If proven effective in humans, it could offer a new paradigm for sepsis management, moving beyond simply treating the infection and supporting failing organs. By directly targeting a key driver of the detrimental inflammatory response, this approach could potentially:
- Reduce Mortality Rates: By mitigating the widespread tissue damage and organ dysfunction associated with sepsis.
- Shorten Hospital Stays: Leading to quicker recovery and reduced healthcare costs.
- Improve Long-Term Outcomes: Potentially lessening the incidence of post-sepsis complications and long-term disability.
- Offer Hope for Refractory Cases: Providing a therapeutic option for patients who do not respond adequately to current treatments.
The scientific community will be closely watching the progress of Eliaz Therapeutics as they strive to translate these encouraging pre-clinical results into a life-saving therapy for one of the world’s most pressing public health challenges. The journey from laboratory discovery to widespread clinical application is often long and arduous, but the potential rewards in combating sepsis make this endeavor critically important.







