Mental Health After A Disaster
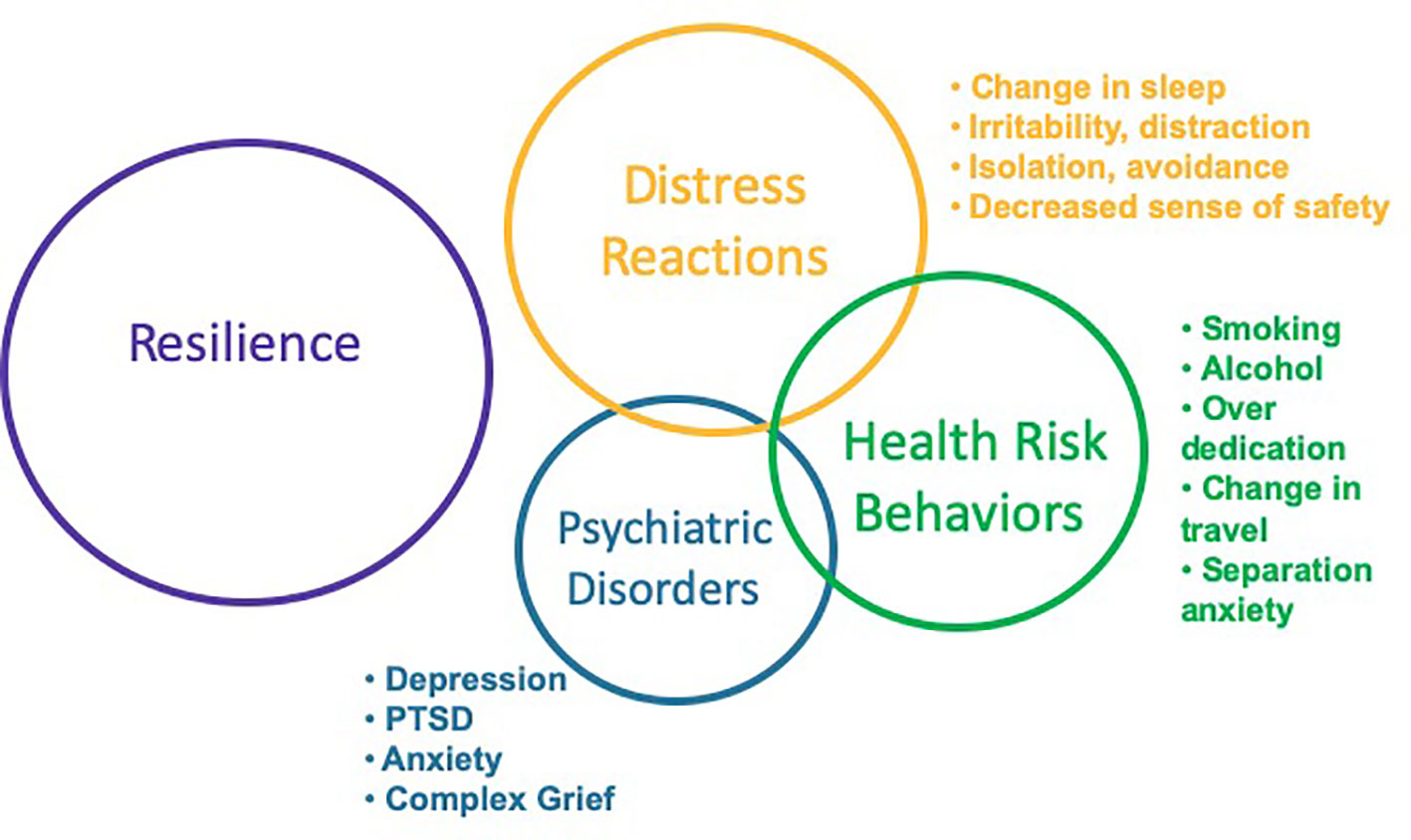


Mental Health After Disaster: Navigating Trauma and Building Resilience
Disasters, whether natural like hurricanes, earthquakes, and floods, or human-made such as acts of violence, industrial accidents, or pandemics, inflict profound and multifaceted impacts on individuals and communities. Beyond the immediate physical devastation and loss of property, the mental and emotional toll can be extensive and long-lasting. Understanding the psychological sequelae of disaster exposure is crucial for effective intervention, support, and fostering resilience. This article delves into the common mental health challenges experienced after disasters, the underlying mechanisms of trauma response, and evidence-based strategies for recovery and long-term well-being.
The immediate aftermath of a disaster is characterized by acute stress reactions. Individuals may experience shock, disbelief, and a sense of unreality. Hypervigilance, difficulty concentrating, sleep disturbances, and intrusive thoughts or memories are common. These reactions are often a normal response to an abnormal situation. However, for some, these acute symptoms can persist and evolve into more significant mental health conditions. The disruption of daily routines, loss of social support networks, and uncertainty about the future can exacerbate these initial reactions. Survivors may also grapple with feelings of guilt, shame, or anger, particularly if they feel they could have done something differently or if they witness the suffering of others. The sheer overwhelm of the situation can lead to a sense of helplessness and a loss of control, which are significant contributors to psychological distress.
As the acute phase subsides, more complex mental health issues can emerge. Post-Traumatic Stress Disorder (PTSD) is a well-documented consequence of disaster exposure. PTSD is characterized by the re-experiencing of the traumatic event through flashbacks and nightmares, avoidance of reminders of the trauma, negative alterations in cognitions and mood, and alterations in arousal and reactivity. For instance, survivors of a major earthquake might experience recurring images of collapsing buildings, avoid news reports about seismic activity, develop a pervasive sense of dread, and become easily startled by loud noises. The severity and duration of disaster exposure, the degree of personal threat experienced, and the presence of pre-existing vulnerabilities can all influence the likelihood of developing PTSD.
Beyond PTSD, other anxiety disorders are frequently observed. Generalized Anxiety Disorder (GAD) can manifest as persistent and excessive worry about a range of issues, including personal safety, the well-being of loved ones, and the future. Panic disorder, characterized by recurrent, unexpected panic attacks, can also be triggered by the intense fear and arousal associated with disaster events. The fear of future disasters can lead to anticipatory anxiety, creating a constant state of unease. Social anxiety can emerge or worsen as individuals feel self-conscious about their appearance, their losses, or their emotional state in social interactions, especially in the context of community rebuilding.
Depression is another prevalent mental health consequence of disaster. Survivors may experience persistent sadness, loss of interest or pleasure in activities, changes in appetite and sleep, fatigue, feelings of worthlessness, and difficulty concentrating. The loss of loved ones, homes, jobs, and a sense of normalcy can all contribute to profound feelings of grief and despair. Complicated grief, a more prolonged and intense form of grief that interferes with daily functioning, can also arise when the loss is particularly overwhelming or when the deceased was a primary source of support. The existential questions raised by a disaster – the fragility of life, the perceived injustice of events – can also contribute to depressive symptoms.
Substance use disorders can emerge or escalate as individuals attempt to cope with the psychological distress. Alcohol and drugs may be used as a form of self-medication to numb emotional pain, reduce anxiety, or facilitate sleep. This can lead to a dangerous cycle of addiction, further complicating recovery and hindering the development of healthier coping mechanisms. The availability of substances in disaster-affected areas can also increase the risk of initiation or relapse for individuals with a history of substance abuse.
Children and adolescents are particularly vulnerable to the mental health impacts of disasters. Their developing brains and emotional regulation skills make them more susceptible to the effects of trauma. Common reactions in children include regression to earlier behaviors (e.g., bedwetting, thumb-sucking), increased clinginess, nightmares, irritability, and difficulty concentrating in school. Younger children may express their distress through play or behavioral changes, while older children and adolescents may exhibit more overt signs of anxiety, depression, or anger. The disruption of family routines and the stress experienced by caregivers can further impact a child’s well-being.
The mechanisms underlying these mental health responses are rooted in the body’s natural stress response. The fight-or-flight response, mediated by the sympathetic nervous system and the release of stress hormones like cortisol and adrenaline, is activated in the face of danger. While adaptive in the short term, prolonged activation or dysregulation of this system can lead to neurobiological changes that underpin mental health disorders. The hippocampus, responsible for memory consolidation, and the amygdala, involved in processing fear, can be significantly impacted. Impaired neurogenesis and alterations in neurotransmitter systems can contribute to persistent anxiety and depressive symptoms. Furthermore, social and environmental factors play a critical role. Loss of social support, economic hardship, displacement, and exposure to ongoing stressors in the post-disaster environment can all impede recovery.
Building resilience is a critical component of mental health recovery after a disaster. Resilience is not the absence of distress, but rather the capacity to adapt well in the face of adversity, trauma, tragedy, threats, or significant sources of stress. Several factors contribute to individual and community resilience. Strong social support networks, both familial and community-based, are paramount. The ability to connect with others, share experiences, and receive practical and emotional support can significantly buffer the impact of trauma. Active coping strategies, such as problem-solving, seeking information, and engaging in enjoyable activities, are more effective than passive coping mechanisms like avoidance or substance use.
Psychological first aid (PFA) is an evidence-based approach designed to provide immediate, humane, and helpful support to people experiencing disaster-related distress. PFA focuses on meeting basic needs, providing emotional support, facilitating connection with social supports, and promoting adaptive coping. It is not a replacement for therapy but serves as a crucial initial intervention to stabilize individuals and connect them with appropriate services.
Trauma-informed care is essential in all aspects of disaster response and recovery. This approach recognizes the pervasive impact of trauma and emphasizes safety, trustworthiness, collaboration, empowerment, and cultural humility. It involves understanding the signs and symptoms of trauma, avoiding re-traumatization, and creating environments that promote healing and well-being.
Evidence-based psychotherapies play a vital role in treating the specific mental health conditions that emerge after disasters. Cognitive Behavioral Therapy (CBT) is highly effective in treating PTSD and anxiety disorders. CBT helps individuals identify and challenge negative thought patterns and develop more adaptive coping behaviors. Trauma-focused CBT (TF-CBT) is specifically designed for children and adolescents and incorporates elements of psychoeducation, relaxation techniques, and gradual exposure to trauma memories. Eye Movement Desensitization and Reprocessing (EMDR) is another effective therapy for PTSD, which involves processing traumatic memories through bilateral stimulation, such as eye movements.
Medication can also be a valuable tool in managing the symptoms of PTSD, depression, and anxiety. Selective Serotonin Reuptake Inhibitors (SSRIs) are commonly prescribed for these conditions. However, medication should be used in conjunction with psychotherapy and under the guidance of a qualified healthcare professional.
Community-based interventions are crucial for fostering collective resilience. This can include establishing mental health support groups, providing access to mental health professionals, offering stress management workshops, and facilitating community healing activities. Empowering local leaders and organizations to take ownership of mental health initiatives can enhance their sustainability and effectiveness. Public health campaigns that normalize seeking mental health support and reduce stigma are also essential.
Disaster preparedness and planning should include robust mental health components. This involves training first responders and community members in mental health first aid, developing protocols for providing psychological support in the immediate aftermath, and establishing long-term mental health service delivery systems. Investing in mental health infrastructure and ensuring adequate funding for disaster mental health services are critical for effective response and recovery. The long-term impacts of disasters necessitate a sustained commitment to mental health support, recognizing that healing and recovery are often non-linear processes. Early identification of at-risk individuals and prompt access to appropriate interventions are key to mitigating the enduring psychological consequences of disaster.





